
Jamaica Hospital Integrative Health Learning Collaborative Case
The Integrative Health Learning Collaborative sought to improve the delivery of whole-person care and make integrative health routine and regular in primary care. During the learning collaborative, Jamaica Hospital Medical Center delivered integrative health to more patients, moved the mindset from sick care to wellness and health and showed that it is possible to deliver integrative health to underserved patients in urban health care settings.
Introduction
[ultimate_heading main_heading=”THE BURDEN OF CHRONIC DISEASE” heading_tag=”h3″ main_heading_color=”#0f6378″ alignment=”left” main_heading_style=”font-style:italic;,font-weight:bold;” main_heading_font_size=”desktop:20px;” main_heading_margin=”margin-bottom:20px;”][/ultimate_heading]Six in 10 adults in the U.S. have at least one chronic disease, and four in 10 have two or more, according to the CDC.1 People in underserved communities bear far more of the burden of chronic disease than people in more affluent communities.
The COVID-19 pandemic emphasized these health and health care disparities. More people in underserved communities, especially those from racial and ethnic minority groups, got sick or dyed or were at higher risk of getting sick and dying from COVID-19 compared to the general population.
Even before the pandemic, primary care providers struggled to find the time, tools and resources to help patients with chronic diseases—whether affluent or underserved—improve their health and wellbeing. Yet, most chronic diseases seen in primary care can be prevented, managed or even reversed by addressing their underlying social and behavioral determinants.
BETTER WAY TO MANAGE CHRONIC DISEASE
Whole-person care and integrative health focus on helping patients achieve health and wellbeing, not just on the treatment of disease, illness and injury. It is a better way to manage chronic disease because it addresses all the factors that impact health and healing:
- Medical treatment
- Mental health
- Personal behaviors and lifestyle
- Social determinants of health
- Personal determinants of healing
Integrative primary care providers use all proven approaches:
- Evidence-based conventional medicine
- Non-drug treatments (including complementary and alternative medicine)
- Self-care
They focus on what matters most to each person and establish trusting, ongoing relationships to help patients heal.
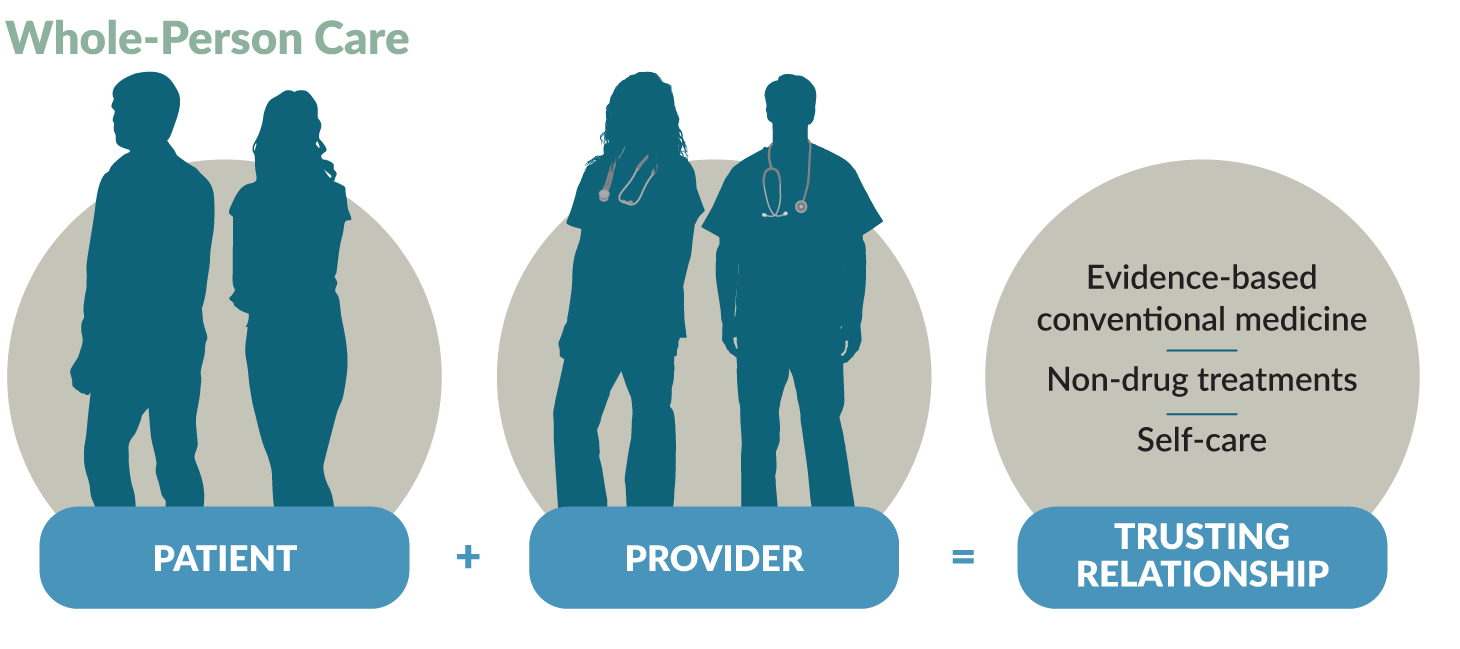
Whole-Person Care
Helps patients achieve health and wellbeing:
Integrative primary care providers use a person-centered, relationship-based approach to integrate self-care with evidence-based conventional medicine and non-drug treatments. They consider all factors that influence healing:
- Medical treatment
- Mental health
- Personal behaviors and lifestyle
- Social determinants of health
- Personal determinants of healing
Uses proven approaches:
Integrative primary care providers coordinate the delivery of evidence-based conventional medicine and non-drug treatments and self-care:
- Conventional medicine is the delivery of evidence-based approaches for disease prevention and treatment currently taught, delivered and paid for by the mainstream health care system.
- Non-drug treatments focus on non-pharmacological approaches to care and include what is sometimes called complementary and alternative medicine (CAM).
- Self-care is all the evidence-based approaches that individuals can engage in to care for their own health and wellbeing. Self-care promotes healthy behaviors and a healthy lifestyle to enhance health and healing. Approaches focus on the connection between the body, the mind the spirit and behavior, and cover food, movement, sleep, stress, substance use and more. Improving one area can influence the others and benefit overall health.
Goes beyond the doctor’s office to consider context:
Whole-person care is framed by each person’s social and personal context:
- Social determinants of health are the conditions in the places where people live, learn, work and play that affect health and quality of life.
- Personal determinants of healing are those personal factors which influence and promote health and healing. These include the physical, environmental, lifestyle, social, emotional, mental and spiritual dimensions which are connected and must be balanced for a happy and fulfilled life.
- Health Coaching is a delivery method for whole-person care. Health coaches use their expertise in human behavior to help individuals set and achieve health goals. They are an increasingly important component of whole-person care teams.
Providers work with patients to create a personalized health plan based on the person’s needs and preferences. To do this, they use free tools such as:
- The PHI (Personal Health Inventory), which assesses the person’s meaning and purpose in life, current health and readiness for change. Patients complete this before or during a primary care visit that integrates health and wellbeing.
- The HOPE (Healing Oriented Practices & Environments) Note, a patient-guided process to identify the person’s values and goals in life and for healing so the provider can assist them in meeting those goals with evidence and other support.
Whole-Person Care Works
Evidence shows that whole-person care is effective in meeting the quadruple aim of:
- Better outcomes
- Improved patient experience
- Lower costs
- Improved clinician experience
Read more about the evidence supporting whole-person care.
THE INTEGRATIVE HEALTH LEARNING COLLABORATIVE
The Integrative Health Learning Collaborative sought to better manage chronic disease by addressing social and behavioral determinants of health to:
- Improve the delivery of whole-person care
- Make integrative health routine and regular in primary care
Seventeen clinics participated in the learning collaborative, held from October 2020 to September 2021. The Family Medicine Education Consortium and Samueli Integrative Health Programs sponsored the learning collaborative, which was funded by a grant from The Samueli Foundation.
Read more about the Integrative Health Learning Collaborative.
THE CHALLEGNE
[ultimate_heading main_heading=”FINDING A BETTER WAY TO CARE FOR UNDERSERVED PATIENTS” heading_tag=”h3″ main_heading_color=”#0f6378″ alignment=”left” main_heading_style=”font-style:italic;,font-weight:bold;” main_heading_font_size=”desktop:20px;” main_heading_margin=”margin-bottom:20px;”][/ultimate_heading]Jamaica Hospital Medical Center is a 404-bed hospital that is part of MediSys Health Network, a not-for-profit integrated healthcare delivery system that is based in Queens, NY. Most of the 1.2 million patients the hospital serves each year are uninsured or underinsured with little access to quality health care. Patients are culturally diverse, primarily Black and Hispanic, with a significant number of immigrants, many undocumented.
MediSys Health Network supports Jamaica Hospital Medical Center and Flushing Hospital Medical Center. It also includes 16 neighborhood-based family health care centers, a nursing home and a center for traumatic brain injury. The network has 502 physicians in more than 60 specialties, 6,588 staff and an annual budget of approximately $1.7 billion.
Jamaica Hospital Medical Center’s Jamaica Family Medicine Center is a residency clinic that is affiliated with the Albert Einstein College of Medicine. More than 20 providers handle about 1,800 patient visits each month.
AN INTEGRATIVE APPROACH TO PATIENT CARE
Alan R. Roth, DO, FAAF, is one of the providers using integrative health to provide better care to his patients and the leader of the effort to implement integrative health in primary care across the MediSys Health Network. Dr. Roth is the chairman of the Department of Family Medicine, Ambulatory Care and Community Medicine and chief of the Department of Integrative Pain and Palliative Care Medicine at the MediSys Health Network, Flushing Hospital Medical Center and Jamaica Hospital Medical Center.
In 2018, Dr. Roth formed an informal group of family medicine and ambulatory providers at Jamaica Family Medical Center to discuss integrative health. They began implementing integrative approaches to patient care, with an emphasis on nutrition, exercise and prevention.
“I don’t go through a visit with a patient without addressing at least one component of wellness and integrative health. Yoga is my first-line therapy for back pain now,” he says.
“Keeping patients healthy is essential to the health of the hospital.”
Along with providing better care to underserved patients, the integrative health approach helps the hospital achieve financial sustainability. “About 50% of our income is in globally capitated lives where we are paid a flat rate and take the full risk on about 200,000 people,” says Dr. Roth.
Senior hospital administrators began supporting work to expand integrative health after Dr. Roth explained how investing in this would reduce:
- Emergency department visits
- Hospital admissions and re-admissions
- Testing
- Over-utilization of services
- Over-prescribing of drugs
A FOCUS ON WHAT MATTERS TO THE PATIENT
Kamica Lewis, DO, assistant program director of the Family Medicine Residency Program at Jamaica Hospital Medical Center, is working closely with Dr. Roth. They realized their mutual interest in integrative health during one of her training sessions in mindfulness and emotional intelligence for hospital leaders.
Family Medicine Physician Discovers Integrative Health
Like many family medicine physicians, Kamica Lewis, DO, was idealistic when she joined Jamaica Hospital Medical Center. “I wanted to save the world and really take care of my patients,” she says. “About two years in, I realized I was just giving patients pills. I wasn’t getting the results I wanted and I was being pushed to see patients in a short period of time.”
Dr. Lewis began feeling burnout. In her search for an evidence-based solution, she found and took a class in mindfulness-based stress reduction. “This was life-changing for me. I was excited to go to work again,” she says. Next, Dr. Lewis achieved certification in mindfulness and emotional intelligence from the Search Inside Yourself Institute and completed a fellowship in integrative medicine at the University of Arizona Andrew Weil Center for Integrative Medicine.
Along with using integrative health with her patients, Dr. Lewis teaches this approach to residents. Also, she teaches mindfulness to physicians and residents and mindfulness and emotional intelligence to hospital leaders.
By focusing on what matters to the patient, integrative health engages patients. “If you have an understanding of where the patient is coming from and approach this as a partnership, the patient feels like they’re being heard and understood,” says Dr. Lewis. Patients who feel like their primary care provider is listening to them are more receptive to discussing their whole health and the small changes they can make to begin to improve their health and wellbeing.
“You get a lot more buy-in by helping patients find solutions and taking a few extra minutes to explain things instead of just telling them what they need to do.”
THE INTEGRATIVE HEALTH PLAN
MediSys Health Network’s plan for integrative health started with educating physicians and residents about integrative health. Current steps are:
- Changing the philosophy of care from sick care to focusing on health and wellbeing
- Offering integrative health group visits and other integrative health services
The last part of the plan will be creating urban integrated health centers of excellence that are based in the community and open to everyone. They will focus on primary care and fully integrate mental and physical health. Integrative health services will also be available to patients in traditional primary care practices.
Planned features of the centers include:
- Clinical offices
- A gym where people can exercise and take classes such as yoga and tai chi
- A demonstration kitchen where nutritionists and chefs will teach healthy cooking
Dr. Roth also hopes to rent space in the building to a healthy grocery store and to have a community garden. Plans to open the centers were delayed due to the COVID-9 pandemic. With funding from philanthropy, MediSys Health Network will modify existing buildings or build new centers. Until this can be done, more integrative health services will be added within current family medicine sites.
WORK DURING THE INTEGRATIVE HEALTH LEARNING COLLABORATIVE
[ultimate_heading main_heading=”USING INTEGRATIVE HEALTH TO CARE FOR MORE UNDERSERVED PATIENTS” heading_tag=”h3″ main_heading_color=”#0f6378″ alignment=”left” main_heading_style=”font-style:italic;,font-weight:bold;” main_heading_font_size=”desktop:20px;” main_heading_margin=”margin-bottom:20px;”][/ultimate_heading]During the Integrative Health Learning Collaborative, the integrative health team at Jamaica Family Medicine Center delivered integrative care to more patients and developed processes for tracking and documenting integrative health visits. The team also continued work to change the mindset at MediSys Health Network from sick care to wellness and health.
THE INTEGRATIVE CARE TEAM AND PROCESS
The integrative care team at Jamaica Family Medicine Center is comprised of:
- Seven faculty members
- One other physician
- Six family medicine residents
- Two patient navigators/health coaches
- An integrative health coordinator
- A nutritionist
- A psychologist
- An administrator
The physicians and residents identify and treat patients who would benefit from integrative health services, conduct integrative health visits and track patient progress. Patient navigators/health coaches do the PHI with patients, serve as health coaches and arrange appointments and follow-up contacts.
Edwin Castano, QMI (qualified medical interpreter) is one of the patient navigators. The child of Spanish speaking immigrants who grew up a few blocks from the hospital, Edwin understands the needs of patients. Doing the PHI with patients over the telephone enables him to develop “meaningful connections” with them.
Most visits focus on a part of the HOPE Note that’s most relevant to the patient’s needs. Dr. Lewis, for example, asks some of the general questions to gain an understanding of the patient and then focuses on finding integrative health solutions for his/her current needs.
“Asking every single question is impossible in a 15- to 20-minute session,” says Dr. Lewis. “If we think the patient would benefit from more time, we can schedule a 40-minute visit.” In reality, however, while administrators have approved the longer integrative health visits, providers rarely had time for this during the worst of the pandemic. By fall 2021, they were able to do more longer integrative health visits.
The integrative health coordinator coordinates appropriate health care and social services for patients and provides support with health care-related needs. The nutritionist provides nutritional advice and support and the psychologist provides behavioral health and mental health support services. The administrative assistant focuses on data, reporting and team meetings and communications.
The Resource Library
The Jamaica Family Medicine Center developed an integrative health resource library for patients with content on mindfulness-based stress reduction, healthy eating and more. Most resources are electronic, however, print handouts are available for patients who don’t have a smart phone (about five percent of the center’s patients).
Most of the resources, as well as information about integrative health services such as nutrition and group visits, are available on Epic (the hospital’s electronic health record system). A monthly newsletter keeps providers updated on new and existing resources.
Patient Case: Integrative Health Relieves Depression
During her annual physical exam, 20-year-old Alicia (not her real name) admitted that she was feeling overwhelmed by school and life and was having episodes of depression. Alicia is under pressure to do well in school while also working part-time taking care of young kids. Also, her mother expects Alicia to help out at home and her brother and mother don’t give her enough space or privacy to do her schoolwork.
Alicia doesn’t want to interact with family or friends during episodes of depression and she lacks motivation to even get out of bed in the morning. She misses school and work.
What matters most to Alicia, uncovered during an integrative health visit, is having the energy and motivation to get out of bed and be productive.
The provider reassured Alicia that being overwhelmed and depressed are common, and that the Jamaica Family Medical Center could support her. They discussed medications, breathing exercises, exercise and diet. Alicia wanted a more natural alternative to an SSRI so the provider suggested an over-the-counter SAMe (S-adenosyl-methionine), a natural compound in the body that helps produce and regulate hormones and maintain cell membranes.
At the six-week follow-up visit, Alicia said she felt much better. The SAMe helped her feel more energetic and more motivated to get things done. She was no longer missing school or work.
Alicia continued to feel better. At the next visit eight weeks later, she noted that she had joined a gym and looked forward to working out. She was eating healthier and had lost some weight.
Balancing school and work and home life was much easier now. Alicia’s family is respecting her space, which has helped decrease her anxiety and feeling overwhelmed. She stopped the SAMe two weeks earlier and feels fine. She is now on a healing journey that taps into her own self-care.
EVALUATING WHOLE-PERSON CARE
Jamaica Hospital Medical Center evaluated its use of integrative health for practice and clinical improvement. They used the Plan-Do-Study-Act (PDSA) cycle and the McKinsey 7S model of change management to plan and manage implementation and to evaluate their changes and plan next steps to expand the delivery of integrative health.
Read more about PDSA cycles and the McKinsey 7S model of change management.
Here is what Jamaica Hospital Medical Center did.
KEY RESULTS
[ultimate_heading main_heading=”CLOSING THE DISPARITIES GAP, CHANGING THE MEDICAL MINDSET AND SHOWING WHAT IS POSSIBLE” heading_tag=”h3″ main_heading_color=”#0f6378″ alignment=”left” main_heading_style=”font-style:italic;,font-weight:bold;” main_heading_font_size=”desktop:20px;” main_heading_margin=”margin-bottom:20px;”][/ultimate_heading]Jamaica Hospital Medical Center reported the following accomplishments related to integrative health before and during the Integrative Health Learning Collaborative.
CLINIC HIGHLIGHTS
Primary care providers treated more underserved patients with whole-person care and integrative health, aiding in closing the disparities gap.
The integrative health team is using the HOPE Note process and tools for discussions about the patient’s values and goals and ways to help each patient meet those goals. “Integrative health gives patients voice and choice in their care. The patients set priorities for their health instead of being told by a provider what to do,” says Castano.
During the Integrative Health Learning Collaborative, the team introduced integrative health group visits for patients with chronic diseases and expanded the role of patient navigators like Castano to include health coaching. They plan to add acupuncture and massage to their services through contracts with local schools training those providers.
“Patients love the extra engagement in integrative health. They feel that we care what’s going on and that they’re not just a number.”
Thirteen staff members completed training in group visits, which currently focus on pain management or health and wellness empowerment. “Patients tend to learn and be more inspired from each other than from just speaking to a physician,” says Dr. Lewis who led the introduction of group visits and facilitated one group.
Also, group visits help combat the epidemic of loneliness that was exacerbated by COVID-19.
“Group visits show patients that they’re not alone,” says Dr. Roth. Decreasing loneliness improves health outcomes, adds Dr. Lewis.
Providers facilitated the group visits, with the help of patient navigators and the administrative assistant. Each group met for 60 to 90 minutes weekly for six weeks and focused on a different topic each week. The facilitator introduced the topic then led an activity and the discussion. At the end of each session, patients had homework, something they choose or agreed to do before the next session to be healthier.
“Often, we say a few words and then the patients start teaching each other and supporting each other,” says Dr. Lewis. “It gives people hope and builds buy-in when patients feel they have peers to be accountable to. They want to step up and do what they said they would do.”
As a co-facilitator in the group visits, Castano serves as a host, “making everyone feel at home” and participates in the discussions. “Group visits create community bonds in a safe space. Watching patients create those bonds and become friends with each other was amazing,” he says.
Learn more about group visits:
Chronic Disease Management with Group Visits (PDF), is a case study on how to promote healthy behaviors among patients with chronic diseases
A health system is changing the mindset from sick care to wellness and health.
Along with changing clinical practice, Dr. Roth and hospital leaders are transforming the MediSys Health Network to focus on integrative health and use fewer drugs to treat patients.
“We’re changing the philosophy of care and cutting down on the use of pharmaceuticals.”
Residents and attending physicians are seeing the benefits of using the HOPE Note in providing better care to patients. Engaging residents in integrative health is especially important in changing mindsets at MediSys Health Network and more broadly.
“Residents are like sponges. What you teach them during these years is very impactful,” says Dr. Lewis. “We’re teaching them to give the best care to underserved populations. When they graduate, they’ll be able to become leaders in integrative health and create change wherever they go.”
Resident training at Jamaica Hospital Medical Center includes monthly integrative medicine grand rounds and a monthly noon conference for residents and faculty. Each year, three residents are enrolled in the University of Arizona Integrative Medicine in Residency certificate program.
Much of the learning is hands-on through discussions of using the PHI and the HOPE Note with patients and how this is different than usual care. Also, residents learn how to collaborate with other professionals, such as nutritionists and the social worker.
Jamaica Hospital Medical Center embedded integrative health tools such as the PHI and the HOPE Note into Epic.
Conducting and tracking integrative health visits is easier now that integrative health tools are part of Epic. Physicians, residents and health navigators have access to tools, and integrative health visits can be documented like a traditional medical visit.
Tools that are now embedded in Epic are:
- HOPE Note
- PHI
- PROMIS-10
- CDC Healthy Days Measures
The integrative health team worked with the hospital’s IT department to develop a tracking system and data reports for use in monitoring the effects of integrative health interventions. Leaders troubleshoot problems with providers.
Integrative health became a routine part of care for COVID-19 patients with ongoing symptoms.
To help patients recover from ongoing COVID symptoms, Jamaica Hospital Medical Center established a long-COVID integrative health clinic comprised of a primary care physician, a pulmonologist, a mental health provider and other specialists. The primary care physician uses the PHI and the HOPE Note to assess each patient and to develop an individualized integrative health care plan.
The integrative health care plan is based on the patient’s symptoms, life goals, medical needs and lifestyle. The team uses a combination of symptom management and self-care to help patients recover from COVID. Treatments include an anti-inflammatory diet, breathing exercises, exercise and a mindfulness plan, such as yoga, journaling, meditation or guided imagery. Medications are used when needed and appropriate. Recently, the clinic published a peer-reviewed article on the use of integrative health for treatment of long-COVID. 2
Jamaica Hospital Medical Center demonstrated the importance of delivering, and the ability to deliver, integrative health in urban health care settings.
“Being able to implement an integrative health approach is more challenging here than anywhere. If we can make this happen in one of the poorest hospitals in New York, anyone can,” says Dr. Roth.
Adds Castano, “We’re really making a different in our patients’ lives. We are creating stronger bonds, one patient at a time.”
LEARNING COLLABORATIVE HIGHLIGHTS
The integrative health team at Jamaica Hospital Medical Center reported the following benefits of participating in the Integrative Health Learning Collaborative.
The integrative health effort regained momentum lost due to COVID-19.
Being part of the Integrative Health Learning Collaborative helped the integrative health team focus on their goals: educating physicians and residents about integrative health, implementing integrative health services and ultimately, creating integrative health centers. The team also developed a more organized approach to implementing integrative health.
“We were so motivated before COVID but we were exhausted in the past year and a half. The learning collaborative helped us reset and refocus on our goals.”
Learning from other clinics participating in the Integrative Health Learning Collaborative was valuable.
Meeting other people who are also engaged in implementing integrative health encouraged and challenged the integrative health team at Jamaica Hospital Medical Center. Also, the integrative health team learned from clinics that had more advanced integrative health programs. One key insight was the need to gather resources early before implementing integrative health programs.
“We’re happy that we did it,” says Dr. Roth. “We have gotten a lot of our folks excited about this approach to wellness and health.”
Members of the integrative health team benefitted personally from participating in the Integrative Health Learning Collaborative.
Dr. Roth, Dr. Lewis and Castano all benefitted personally from participating in the Integrative Health Learning Collaborative. Dr. Roth says that participating has “speeded up the knowledge” of members of his team, giving him more help in implementing integrative health at Jamaica Hospital Medical Center. “That has taken some of the burden of implementation off of me,” he says.
For Dr. Lewis, practicing integrative health is helping her take care of her patients the way she wanted to when she was an idealistic resident. Now she can focus on helping her patients achieve health and wellbeing.
Castano built his skillset. “I’ve been helping patients navigate the health system. Now I also help them navigate their health choices,” he says. His expanded role is “very satisfying and rewarding.”
Key Insights for Implementing Integrative Health
Buy-in from leadership is essential. Dr. Roth was able to convince senior hospital administrators to support integrative health by demonstrating how it would lower costs and improve patient care at Jamaica Hospital Medical Center. “Get the right people in the room and give presentations on integrative health and why an integrative health approach is important to your organization,” he says.
Learn more about the Evidence Supporting Whole-Person Care.
Create and share goals and define roles and responsibilities. Implementing integrative health takes time and effort. Create goals that providers and administrators agree upon to facilitate the work. Define roles and roles and responsibilities of the team members who will be implementing integrative health.
For example, initially, providers were doing the PHI with patients and entering data into Epic, but the providers didn’t have time to complete the PHI in a visit. The team trained patient navigators to do the PHI and enter the data before the visit. Providers were very happy with this and were able to focus on the HOPE Note discussion and development of a personalized health plan during the visit.
Develop resources for patients early and make it easy for providers to access them.
Providers need health and wellness resources to share with their patients. Develop resources early in the implementation of integrative health so that when providers identify a need, they can help their patients.
Current resources at Jamaica Hospital Medical Center include educational tools on diet and education, a YouTube series on integrative health with classes in yoga and tai chi, and group visits. The YouTube integrative health series (scroll down to integrative health) includes videos on yoga, mindful meditation, exercise, nutrition, supplements and more. Dr. Roth recommends including massage therapy and acupuncture, which he plans to add soon. Jamaica Hospital Medical Center made the resources available to providers through Epic and also highlights them in a monthly newsletter.
Work with integrative health schools. Contracting with professional complementary and integrative health schools such as for acupuncture and massage is a cost-effective way to provide these services, especially for low-income or medically underserved patients. These schools provide lower cost care and often have a sliding fee scale. Faculty instructors closely supervise the care.
Find Integrative Health School Clinics by city or state and practice type.
Train family medicine residents in integrative health. Residents can help provide integrative health and when they complete residency, they’ll take integrative health skills with them to wherever they practice medicine. Training methods include grand rounds, conferences, and hands-on learning through doing and discussing integrative health visits.
Minimize primary care provider burden and maximize time for developing the personalized health plan by using other staff to complete the PHI. Jamaica Hospital Medical Center used patient navigators/health coaches to work with patients to complete the PHI before the visit and to enter data into Epic. This freed up the primary care providers to do a HOPE Note discussion and work with each patient on a personalized health plan.
Integrative Health Resources for Patients and Practitioners
Resources for Patients
- Breathwork Pocket Guide (PDF)
- Trying Mind-Body Medicine for Pain
- Guide to Nutrition for Chronic Pain
- Creating Positive Change
- Integrative Health Self-Care Guide
- Many more
Resources for providers
Provider pocket guides including on:
- Acupuncture
- Breathwork Pocket Guide (PDF)
- Depression
- Mediterranean Diet
- Supplements
- Nutritional Counseling
Reports and guides, including:
NCIPH Resources for Patients and the Public
The National Center for Integrative Primary Healthcare is a collaboration of the University of Arizona Andrew Weil Center for Integrative Medicine, the Academic Consortium for Integrative Medicine & Health and the Health Resources and Services Administration.
Patient education materials cover:
- Various health conditions
- Types of integrative therapies.
They’re available online and in print versions.
CHALLENGES
[ultimate_heading main_heading=”NEEDING RESOURCES AND TIME” heading_tag=”h3″ main_heading_color=”#0f6378″ alignment=”left” main_heading_style=”font-style:italic;,font-weight:bold;” main_heading_font_size=”desktop:20px;” main_heading_margin=”margin-bottom:20px;”][/ultimate_heading]Providers need integrative health resources. Providers at Jamaica Hospital Medical Center started doing integrative health visits without having tools and services to help patients. “There was a lot of frustration. Providers found problems but didn’t know where to send patients or what to do,” says Dr. Roth. He recommends putting together a list of resources early when implementing integrative health. The list should start with at least a dozen or so resources for patients, such as educational tools and services.
Providers have limited time for integrative health. Initially, the integrative health team had the providers do the PHI with patients and enter data into Epic, but the providers didn’t have time to complete the PHI in a visit. The team trained patient navigators to do the PHI with patients and enter the date into Epic before the visit. Providers were very happy with this and were able to focus on the HOPE Note discussion and development of a personalized health plan during the visit.
COVID-19 significantly disrupted the integrative health work. From late fall 2020 to March 2021, Jamaica Hospital Medical Center had another COVID surge. Residents and attending physicians who were working in integrative health were deployed back to the hospital again. For a few weeks, patient navigators were assigned to COVID vaccination efforts and were unable to assist with the PHI and other parts of the integrative health program.
NEXT STEPS
[ultimate_heading main_heading=”EXPANDING INTEGRATIVE HEALTH SERVICES” heading_tag=”h3″ main_heading_color=”#0f6378″ alignment=”left” main_heading_style=”font-style:italic;,font-weight:bold;” main_heading_font_size=”desktop:20px;” main_heading_margin=”margin-bottom:20px;”][/ultimate_heading]Jamaica Hospital Medical Center continues to provide integrative health visits and will be expanding the group visits for patients with chronic disease and begin billing for group visits. The integrative health team will engage more providers and some residents in group visits. The team would like to offer both open and closed groups. In the open groups, patients can drop in when they want to.
Learn more about group visits:
Chronic Disease Management with Group Visits (PDF), is a case study on how to promote healthy behaviors among patients with chronic diseases
Group visits, in person and virtual, are billable if the provider does a brief targeted physical exam with each patient (five minutes or less) and documentation criteria are met. In the initial group visits, Dr. Lewis focused on learning the process and teaching it to other members of the integrative health team. In future group visits, they will be implementing processes to do billable group visits.
The integrative health team plans to engage more patients in integrative health services by providing more integrative health services virtually. Virtual services will include:
- Guided imagery by Health Journeys
- An integrative health resources page on the family medical center’s website
- Continuing the YouTube integrative health series (scroll down to integrative health).
THE INTEGRATED HEALTH CENTERS
Dr. Roth hopes to be able to open the first MediSys Health Network integrative health centers by the spring of 2023. He is working on obtaining funding to modify existing buildings or build new centers. The integrated health centers will integrate mental and physical health for primary care patients and also offer integrative health services to patients in traditional primary care practices within the MediSys Health Network.
APPENDIX 1
[ultimate_heading main_heading=”EVIDENCE SUPPORTING WHOLE-PERSON CARE” heading_tag=”h3″ main_heading_color=”#0f6378″ alignment=”left” main_heading_style=”font-style:italic;,font-weight:bold;” main_heading_font_size=”desktop:20px;” main_heading_margin=”margin-bottom:20px;”][/ultimate_heading]Evidence from existing whole-person care supports the effectiveness of this model in meeting the quadruple aim:
- Better Outcomes
- Improved Patient Experience
- Lower Costs
- Improved Clinician Experience.
This evidence includes a narrative review of several models of whole-person care and studies illustrate the business case for whole-person models in primary care2 and the models and studies cited in this section.
BETTER OUTCOMES
Whole-person care:
- Increases the ability to manage chronic pain and decreases opioid doses.3
- Improves patient-reported health and wellbeing.4
- Lowers A1c in people with diabetes.5
- Improves medication adherence.6
- Facilitates a healthier lifestyle.7
- Reduces the severity of heart disease.8, 9
- Reduces loneliness among seniors.10
- Lessens symptoms, including pain, depression, low back pain and headaches.11, 12, 13
IMPROVED PATIENT EXPERIENCE
Whole-person care:
LOWER COSTS
IMPROVED CLINICIAN EXPERIENCE
APPENDIX 2
[ultimate_heading main_heading=”PDSA CYCLES AND THE MCKINSEY 7S MODEL OF CHANGE MANAGEMENT” heading_tag=”h3″ main_heading_color=”#0f6378″ alignment=”left” main_heading_style=”font-style:italic;,font-weight:bold;” main_heading_font_size=”desktop:20px;” main_heading_margin=”margin-bottom:20px;”][/ultimate_heading]THE PDSA CYCLE
The PDSA cycle is a tool for documenting change. Clinics participating in the Integrative Health Learning Collaborative planned and tested small changes, learned from the results, and modified the changes as necessary.
PDSA Cycle
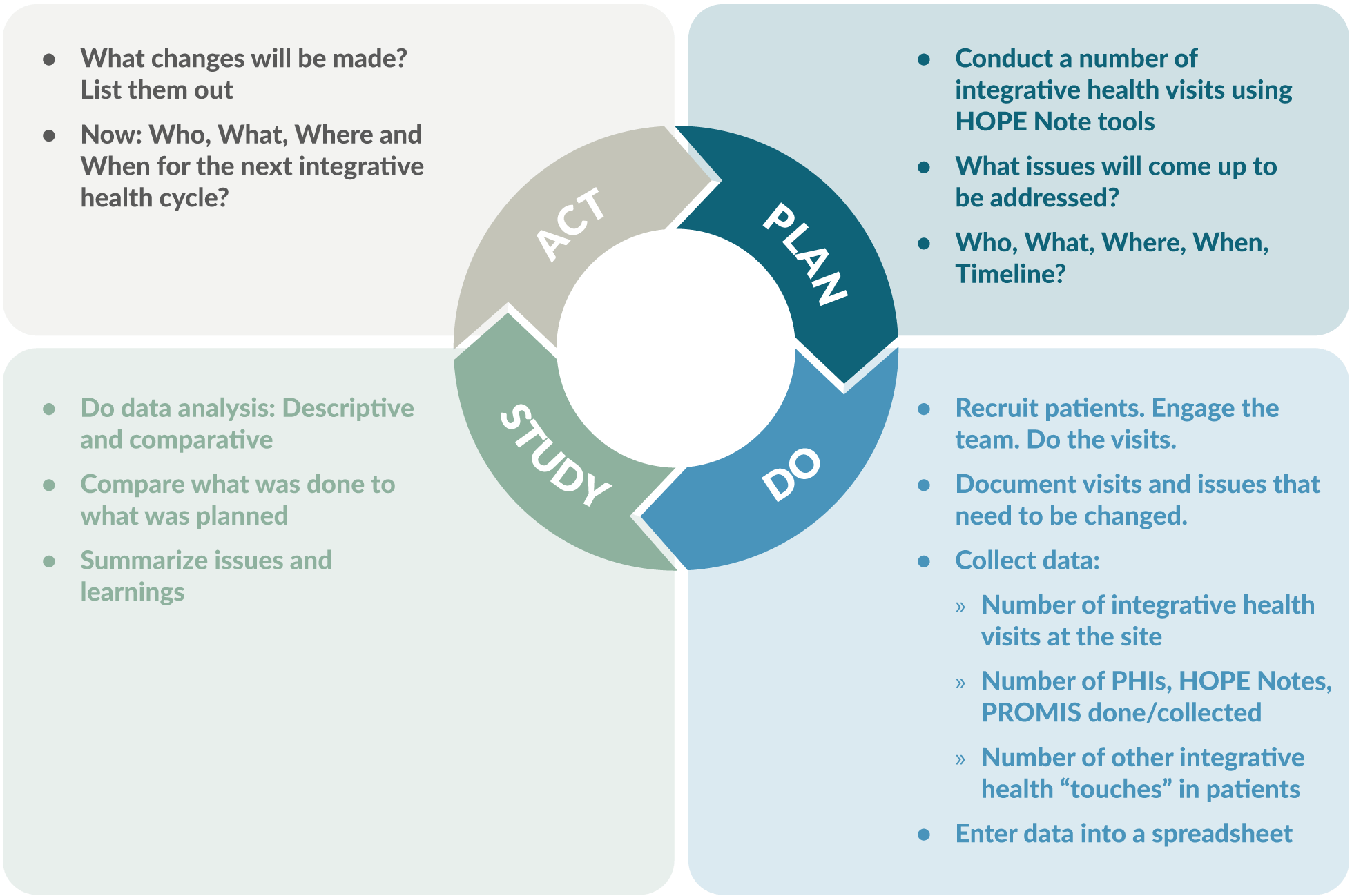
Source: Slide 9, PDSA and 7S Report Outs v1
THE MCKINSEY 7S MODEL OF CHANGE MANAGEMENT
The McKinsey 7S model of change management is a good way to plan and manage implementation of integrative health. The model considers three structural elements: strategy, systems and structure. It also recognizes three “people” elements needed to win the hearts of everyone from front office staff
to the most senior physicians. These include addressing the types of people who are going to lead the change, the skills of the people who will be involved, and the overarching leadership style within the organization. These elements are fuzzier, more intangible, are influenced by corporate culture and are sometimes more difficult to address.
The McKinsey 7S Model of Change Management
Graphic CC-BY 2.5 Wikimedia
Managing change by addressing all these barriers leads to the 7th “S,” creation of shared values underpinning the culture of the group.
Structural and People Elements in the McKinsey 7S Model of Change Management
[su_table responsive=”yes” class=”custom-su-table”]
| Structural Elements: | |
|---|---|
| Strategy: | What do you want to do differently? What will it replace? |
| Systems: | What changes in workflow needs to happen to do the new thing? |
| Structure: | How are you going to set up a new system to kick off and then monitor the initiative? |
| People Elements: | |
| Style: | How are you going to lead the change? |
| Staff: | Who can you enlist who will make it happen? Who do others in your practice look to for guidance? |
| Skills: | Who needs to be trained in the new workflow? What is the training? How can you give them ownership? |
[/su_table]
Addressing all these issues through careful planning will lead to development of the shared values, the commonly accepted standards and norms within the practice that will make the switch to whole-person care a success.
USING THE 7S MODEL TO PLAN IMPLEMENTATION
Substantial planning is necessary to make the change to whole-person care.
Strategy: The obvious changes, as part of this initiative, are to start using the PHI, start conducting integrative visits around the HOPE note, and start setting up a way to monitor both your implementation and the outcomes you’ve settled on. Who is going to do what?
Systems: Careful attention is needed to identify new systems to support whole-person care. Most aspects of the practice will need to be changed in some way, including front-office, billing, and clinical care workflows. Having a Plan B on the shelf will be useful.
Structure: Determine how the roll-out will occur. It may be best to start a pilot project with a single team, carefully chosen for their ability to embrace change. Their success must be carefully monitored so that processes can change when barriers are discovered.
Style: Decide on whether the change to whole-person care will be incremental or dramatic. Decide on who will lead the implementation and how they will approach it. Develop a means of getting staff members excited. Decide how much input the staff will have in the implementation. Set up a rapid cycle quality improvement plan.
Staff: You will need to enlist key people to make your implementations happen and to make it stick. These may be people in key roles, but you will need to identify an opinion leader and a first follower (the first person in the organization to support the opinion leader) for the implementation to be widely adopted.
Skills: Whole-person care requires a new set of skills and new practices. Identify who will need to receive new training and determine how to provide the training.
The McKinsey model is probably well known to most hospital administrators but less known to clinicians and managers. Soon a five-part continuing medical education series for clinicians, staff and managers will be available that explains the HOPE note and introduces integrative health to the team and managing and monitoring the implementation process.
ENDNOTES
- Chronic Disease in America. https://www.cdc.gov/chronicdisease/tools/infographics.htm. Accessed 10/25/21.
- Roth A, Chan PS, Jonas W. Addressing the Long COVID Crisis: Integrative Health and Long COVID. Glob Adv Health Med. 2021; 10:21649561211056597. Published online 2021 Nov 16. doi: 10.1177/21649561211056597. https://www.ncbi.nlm.nih.gov/pmc/articles/PMC8606968/. Accessed 2/24/22.
- Bokhour BG, Hyde J, Zeliadt S, Mohr H. Whole Health System of Care Evaluation – A Progress Report on Outcomes of the WHS Pilot at 18 Flagship Sites. February 18, 2020. Veterans Health Administration, Center for Evaluating Patient-Centered Care in VA (EPCC-VA). https://www.va.gov/WHOLEHEALTH/docs/EPCC_WHSevaluation_FinalReport_508.pdf. Accessed 7/15/21.
- Crocker R, Hurwitz JT, Grizzle AJ, et al. Real-World Evidence from the Integrative Medicine Primary Care Trial (IMPACT): Assessing Patient-Reported Outcomes at Baseline and 12-Month Follow-Up. Evidence-Based Complementary and Alternative Medicine, 2019, Article ID 8595409. https://doi.org/10.1155/2019/8595409. Accessed 7/15/21.
- Hojat M, Louis DZ, Markham FW, Wender R, Rabinowitz C, Gonnella JS. Physicians’ empathy and clinical outcomes for diabetic patients. AcadMed. 2011 Mar;86(3):359-64. doi: 10.1097/ ACM.0b013e3182086fe1. PMID: 21248604. https://journals.lww.com/academicmedicine/Fulltext/2011/03000/Physicians__Empathy_and_Clinical_Outcomes_for.26.aspx. Accessed 7/15/21.
- Zolnierek KB, Dimatteo MR. Physician communication and patient adherence to treatment: a meta-analysis. Med Care. 2009 Aug;47(8):826-34. doi: 10.1097/MLR.0b013e31819a5acc. PMID: 19584762; PMCID: PMC2728700. https://pubmed.ncbi.nlm.nih.gov/19584762/. Accessed 7/15/21.
- Budzowski AR, Parkinson MD, Silfee VJ. An Evaluation of Lifestyle Health Coaching Programs Using Trained Health Coaches and Evidence-Based Curricula at 6 Months Over 6 Years. Am J Health Promot. 2019 Jul;33(6):912-915. doi: 10.1177/0890117118824252. Epub 2019 Jan 22. https://pubmed.ncbi.nlm.nih.gov/30669850/. Accessed 7/15/21.
- Estruch R, Ros E, Salas-Salvadó J, at al. Primary Prevention of Cardiovascular Disease with a Mediterranean Diet Supplemented with Extra-Virgin Olive Oil or Nuts. N Engl J Med 2018; 378:e34. DOI: 10.1056/NEJMoa1800389. https://www.nejm.org/doi/full/10.1056/NEJMoa1800389. Accessed 7/15/21.
- Ornish D, Scherwitz LW, Billings JH, et al. Intensive Lifestyle Changes for Reversal of Coronary Heart Disease. JAMA, December 16, 1998—Vol 280, No. 23. https://pubmed.ncbi.nlm.nih.gov/9863851/. Abstract accessed 7/15/21.
- Thomas KS, Akobundu U, Dosa D. More Than A Meal? A Randomized Control Trial Comparing the Effects of Home-Delivered Meals Programs on Participants’ Feelings of Loneliness. J Gerontol B Psychol Sci Soc Sci. 2016 Nov;71(6):1049-1058. doi: 10.1093/geronb/gbv111. Epub 2015 Nov 26. PMID: 26613620. https://pubmed.ncbi.nlm.nih.gov/26613620/. Accessed 7/15/21.
- Huston P, McFarlane B. Health benefits of tai chi: What is the evidence? Can Fam Physician. 2016 Nov;62(11):881-890. PMID: 28661865. https://www.cfp.ca/content/62/11/881. Accessed 7/15/21.
- Department of Veterans Affairs. Evidence Map of Acupuncture. 2014. https://www.hsrd.research.va.gov/publications/esp/acupuncture.pdf. Accessed 7/15/21.
- Department of Veterans Affairs. Evidence Map of Mindfulness. 2014. https://www.hsrd.research.va.gov/publications/esp/cam_mindfulness-REPORT.pdf. Accessed 7/15/21.
- Press Ganey. Protecting Market Share in the Era of Reform: Understanding Patient Loyalty in the Medical Practice Segment. White Paper. 2013. http://img.en25.com/Web/PressGaneyAssociatesInc/PerfInsights_PatientLoyalty_Nov2013.pdf?elq=a66e16008286435885d97352358aefd3. Accessed 7/15/21.
- Crocker, R.L., Grizzle, A.J., Hurwitz, J.T. et al. Integrative medicine primary care: assessing the practice model through patients’ experiences. BMC Complement Altern Med 17, 490 (2017). https://doi.org/10.1186/s12906-017-1996-5. Accessed 3/10/21.
- The Impact of Relationship-Based Care. South Central Foundation Nuka System of Care. https://scfnuka.com/impact-relationship-based-care/. Accessed 3/10/21.
- Myklebust M, Pradhan EK, Gorenflo D. An integrative medicine patient care model and evaluation of its outcomes: the University of Michigan experience. J Altern Complement Med. 2008 Sep;14(7):821-6. doi: 10.1089/acm.2008.0154. PMID:18721082. https://deepblue.lib.umich.edu/bitstream/handle/2027.42/63379/acm.2008.0154.pdf;sequence=1 . Accessed 7/15/21.
- Cover Commission. Creating Options for Veterans’ Expedited Recovery: Final Report. January 24, 2020. https://www.va.gov/COVER/docs/COVER-Commission-Final-Report-2020-01-24.PDF. Accessed 7/15/21.
- Sarnat RL, Winterstein J. Clinical and cost outcomes of an integrative medicine IPA. Journal of Manipulative and Physiological Therapeutics. 2004 Jun;27(5):336-347. DOI: 10.1016/j.jmpt.2004.04.007. https://cdn.ymaws.com/nebraskachiropractic.org/resource/resmgr/Docs/Clinical_and_Cost_Outcomes.pdf. Accessed 7/15/21.
- Pruitt Z, Emechebe N, Quast T, Taylor P, Bryant K. Expenditure Reductions Associated with a Social Service Referral Program. Popul Health Manag. 2018 Dec;21(6):469-476. doi: 10.1089/pop.2017.0199. Epub 2018 Apr 17. PMID: 29664702; PMCID: PMC6276598. https://pubmed.ncbi.nlm.nih.gov/29664702/. Accessed 7/15/21.
- Jonk Y, Lawson K, O’Connor H, Riise KS, Eisenberg D, Dowd B, Kreitzer MJ. How effective is health coaching in reducing health services expenditures? Med Care. 2015 Feb;53(2):133-40. doi: 10.1097/ MLR.0000000000000287. PMID: 25588134. https://pubmed.ncbi.nlm.nih.gov/25588134/. Accessed 7/15/21.
- Cherkin DC, Herman PM. Cognitive and Mind-Body Therapies for Chronic Low Back Pain and Neck Pain: Effectiveness and Value. JAMA Intern Med. 2018;178(4):556–557. doi:10.1001/jamainternmed.2018.0113. https://jamanetwork.com/journals/jamainternalmedicine/articleabstract/2673371. Accessed 7/15/21.
- De Marchis E, Knox M, Hessler D, Willard-Grace R, Olayiwola JN, Peterson LE, Grumbach K, Gottlieb LM. Physician Burnout and Higher Clinic Capacity to Address Patients’ Social Needs. J Am Board Fam Med. 2019 Jan-Feb;32(1):69-78. doi: 10.3122/jabfm.2019.01.180104. PMID: 30610144. https://pubmed.ncbi.nlm.nih.gov/30610144/. Accessed 7/15/21.
- Wilkinson H, Whittington R, Perry L, Eames C. Examining the relationship between burnout and empathy in healthcare professionals: A systematic review. Burn Res. 2017 Sep;6:18-29. doi: 10.1016/j.burn.2017.06.003. PMID: 28868237; PMCID: PMC5534210. https://pubmed.ncbi.nlm.nih.gov/28868237/. Accessed 7/15/21.
- Eby D, Ross L. Internationally Heralded Approaches to Population Health Driven by Alaska Native/American Indian/Native American Communities. Institute for Healthcare Improvement 8th annual National Forum, 2016. http://app.ihi.org/FacultyDocuments/Events/Event-2760/Presentation-14234/Document-11589/Presentation_L2_Internationally_Heralded_Approaches_to_Population_Health_driven_by_Alaska_NativeAmerican_IndianNative_American_Communities_Eby.pdf. Accessed 7/15/21.
- Finnegan J. Integrative medicine physicians say quality of life is better. Fierce Healthcare. August 22, 2017. https://www.fiercehealthcare.com/practices/doctorspracticing-integrative-medicine-say-quality-life-better.Accessed 7/15/21.
Topics: Complementary Medicine | Integrative Health
