
A Guide to Optimizing Treatment Through Integrative Health for People Living With Pain
LETTER FROM DR. WAYNE JONAS
Dear Friends,
When I think about chronic pain, I think about my patient Margaret and her back pain. She wasn’t sure how it started – maybe she lifted her grandson wrong, or it was the extra hours on her feet at the shop.
Her doctors prescribed medications and physical therapy. She had X-rays and an MRI, which revealed arthritis in her spine. Then she developed intense sciatica – pain shooting down her leg. She received an injection and a prescription for an opioid medication to take when the pain was unbearable, which was often at night.
Other medications followed – for sleep, for the nerve pain, and finally to lift her mood. By the time she came to me, she was on five medications, including a daily opioid. She could no longer exercise and had gained 50 pounds in the past 10 years. She was miserable. When she didn’t take her opioid, she became agitated and irritable – classic signs of opioid dependence.
My goal in providing you with the information in this paper is to help you avoid the 10 years of misery and pain Margaret experienced. As you’ll read, people with chronic pain need three things:
- a health care team that works together and shares information,
- non-drug approaches to help improve function, cope with the pain as well as reduce it, and
- help managing medications with a goal of getting off or reducing opioid use.
Read on to learn more about these three pillars of pain relief.

Yours in health,
Wayne Jonas, M.D.
PAIN DEFINED
Pain is “An unpleasant sensory and emotional experience associated with actual or potential tissue damage, or described in terms of such damage. It is unquestionably a sensation in a part or parts of the body, but it is also always unpleasant and therefore also an emotional experience.”
When you break your leg, undergo surgery, or burn your hand, you experience pain – acute pain. With treatment and time, the pain usually disappears. But chronic pain is different. It hangs around even after the original illness or injury has improved, reminding you every day that it has no plans to vacate the premises. Technically, chronic pain is diagnosed if it persists three to six months or more after an injury or disease heals. 1
Sometimes there is a clear cause of the pain – such as arthritis – but other times there isn’t a specific trigger or underlying illness or condition. For instance, current science suggests fibromyalgia is a chronic pain condition without a specific cause that is likely related to changes in how the brain processes pain. Sometimes people may feel pain in places distant from where the original injury occurred, something called “referred” pain.
Often, chronic pain begins with an acute pain event. The pain can develop and intensify to become chronic pain. If you have chronic pain, you’re not alone. More than 100 million American adults are estimated to have chronic pain. 3 Chronic pain is one of the most frequent reasons for physician visits, and is among the most common reasons for taking medication. 3
But pain is more than just a physical hurt. It is an unwanted guest that takes over your life, interfering with your ability to work, your relationships, your mental health, and your overall quality of life. 3 It affects your entire being.
For example, those with low back pain are three times more likely to have limited functional ability and four times as likely to suffer psychological distress as those without low back pain. 1 Unfortunately, finding the answer to your pain can feel like searching for a unicorn in a horse stable; the answer may not even live there.
NAVIGATING THE HEALTH CARE SYSTEM TO FIND RELIEF
“While pain care has grown more sophisticated, the most effective care still is not widely available. Some cases of acute pain can be successfully treated but are not; others could be dealt with promptly, but agonizing delays occur. And most people with severe, persistent pain still do not receive – and often are not offered – systematic relief or the comprehensive, integrated, evidence-based assessment and treatment that pain care clinicians strive to provide.”
It takes a village to manage chronic pain – or at least a multidisciplinary team of health care professionals with you (and your own self-care) at its center. 3
Yet one of the things the U.S. health care system as a whole systematically fails at is the provision of such coordinated care. 4 Most care is piecemeal with little communication among providers.
So, people with chronic pain are left to jump from provider to provider, often undergoing unnecessary, costly, duplicative procedures, taking ineffective drugs, and finding their stress and anxiety increasing with every missed opportunity to relieve the pain. Often, they may feel as if they have “failed” and lose hope. In reality, it is the health care system that has failed them.
One reason is that health care providers often dismiss or minimize their patients’ reports of pain – particularly in women and racial and ethnic minorities. 5 Indeed, there is evidence that women are more likely to be prescribed psychological treatments for their pain than men, and are more likely to be viewed as overreacting and exaggerating their pain. 6
Part of the problem is that few doctors receive much training in managing acute and chronic pain. In 2010, for instance, just four of the country’s 104 medical schools required that students take a pain course. Those courses lasted between 1.5 and 13 days. Another 17 medical schools offered optional courses on pain. Most disturbing is that few of the courses dealt with the most effective treatments for pain – a multidisciplinary approach involving medical and behavioral interventions. 7
This leaves people with chronic pain undiagnosed, undertreated, and continually searching for a health care provider who can truly help them. Some pain sufferers give up on health care and never find adequate relief.
The Opioid Epidemic and Pain
The issue of pain has become an almost daily headline given the current opioid epidemic. More than 250 million prescriptions are written for opioids each year, and while the amount of prescription opioids sold nearly quadrupled from 1999 to 2010, the amount of pain Americans reported remained unchanged. 8
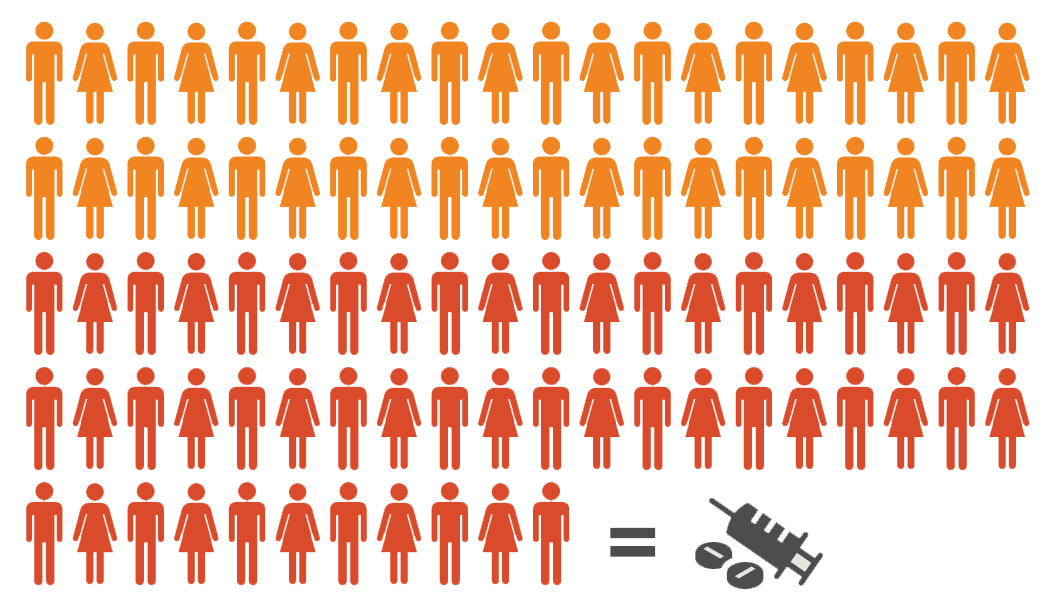
Since 1999, the number of overdose deaths involving opioids (including prescription opioids and heroin) quadrupled, with 91 Americans dying every day from an opioid overdose – more than 40 a day from prescription opioids. 8
There is limited evidence that these hard-hitting drugs are even effective for people with chronic pain like Margaret. 9 They are also highly addictive, and over time, you need higher and higher doses just to get the same relief. 8 They also have serious side effects, including depression, overdose, death, constipation, and withdrawal symptoms when you stop taking them, like the irritability Margaret experienced. Opioids also mask pain rather than address the underlying cause of the pain or enable you to live with the pain and still maintain a functional quality of life. 10
Given all this, in 2017 the Centers for Disease Control and Prevention (CDC) issued new pain management guidelines that specifically state: “In general, do not prescribe opioids as the first-line treatment for chronic pain.” 10
Attempts to reduce opioids, however, without treating the pain, don’t work. Instead, they lead to desperate people who may turn to alternative opioids like heroin, or begin “doctor shopping” to find someone who will write the prescription. That’s why it’s critical to open up to other types of options for reducing pain rather than just reducing the amount of opioids you’re taking.
As this booklet highlights, there are more effective, safer options for pain management.
BUILDING YOUR PAIN MANAGEMENT TEAM
If you’re like most people, the doctor you see most often is your primary care provider, likely a family physician or internist. And that’s certainly the place to start when you’re dealing with pain. Estimates are that primary care physicians treat about half of all people living with chronic pain. 11
However, if your pain remains uncontrolled, it might be time to seek out other practitioners.
In an ideal world, you would have access to a pain management specialist, one board certified in pain management. The American Board of Anesthesiology, the American Board of Psychiatry, the American Board of Neurology, and the American Board of Physical Medicine and Rehabilitation all offer certification after physicians complete a fellowship in pain management.
These physicians typically work in pain management centers and employ a holistic approach to your pain involving medical treatments, psychological counseling, and alternative approaches like those described below.
At the Mayo Clinic, for instance, a three-week patient-oriented pain management program involves physical and occupational therapy, education to better understand your pain, and breathing and meditation exercises to reduce anxiety related to flares. One study of 373 patients who attended the program – half of whom had been taking opioids before enrolling – found significant improvement at six months after the program ended, regardless of the amount of opioid medication they were taking prior to treatment. 12
However, there are a very small number of these physicians and teams available, with one study estimating that just 2 percent of people living with chronic pain receive care from these professionals in a typical month. 11 If there are no pain specialists or teams in your area, ask about telehealth consultations. Studies find that these approaches can be just as effective as in-person visits. 13 14
Other physicians who can provide pain management services include neurologists, orthopedists, anesthesiologists, and rheumatologists. Most of these specialists deal with only one type of pain – the type involving the part of the body they treat. And while a physician should be an important part of your pain management team, you shouldn’t stop there. Studies find that an integrative approach – one that combines conventional medicine with self-care and complementary approaches – is more effective at addressing chronic pain than conventional medicine alone. 15-17
Who is Treating Your Pain?
You may see several physicians as you search for pain relief. These include:
- Primary care physicians. Pain is one of the main reasons people see their primary care physicians. They treat all conditions and should view your condition holistically.
- Pain management specialists. These physicians are often trained in anesthesia with additional training in pain management. They include interventional anesthesiologists, who can implant pumps and other devices to help relieve your pain.
- Neurologists. These physicians focus on the central nervous system. They are most likely to treat neuropathic pain, or pain related to the nerves.
- Orthopedists and sports medicine doctors. These physicians address the skeletal system, including bones, joints, and tendons.
- Physiatrists. These physicians treat a wide variety of medical conditions affecting the brain, spinal cord, nerves, bones, joints, ligaments, muscles, and tendons.
- Rheumatologists. These physicians address the immune system. They are likely to treat people with painful autoimmune diseases like lupus, scleroderma, and fibromyalgia.
Indeed, guidelines from the CDC, American College of Physicians, and other medical organizations recommend starting with non-opioid alternatives as a first-line treatment for chronic pain, including acetaminophen (Tylenol), nonsteroidal anti-inflammatories (i.e., Motrin, Aleve), antidepressants, and anticonvulsants. They also recommend non-medication approaches such as cognitive behavioral therapy – in which you learn to think differently about your pain – physical therapy, movement therapy or exercise, and also complementary approaches such as acupuncture, massage, and chiropractic services. 10 18
WHO ARE THE COMPLEMENTARY PAIN PROVIDERS?
There are other practitioners who can work with you and your physician to relieve your pain. Among them:
- Chiropractors. Chiropractors see approximately 40 percent of people living with chronic pain, with one study finding that about a third of patients with chronic back or neck pain turned to a chiropractor. 11 A survey from Consumer Reports found that 59 percent of people with chronic pain who saw a chiropractor were highly satisfied compared with 34 percent who saw only a primary care physician. 19 20
- Acupuncturists. There is good evidence for the long-term benefit from acupuncture on chronic pain. 21 One study found that acupuncturists treat about 7 percent of chronic pain patients. 11
- Physical therapists. Physical therapists specialize in restoring function to people living with chronic pain. For instance, if you have arthritis of the knee, they work with you to strengthen the muscles that surround the knee, which can help with the pain.
- Massage therapists. About half of those who get a massage every year are doing it for some medical reason – primarily pain relief – or soreness and stiffness. One survey of more than 1,000 adults found that 89 percent believed that massage was effective in reducing pain, with 28 percent stating they used massage therapy for pain relief. 22
- Cognitive behavioral therapists (CBT). Dozens of studies attest to the benefits of this psychological approach, in which you work with a therapist to reframe how you think about and react to your pain. 23
You can learn more about these alternative approaches at www.drwaynejonas.com. Fact sheets include the latest evidence, amenable conditions, precautions, provider training and how to find a provider.
When complementary or alternative approaches are appropriate, it is important to make sure all of your providers are communicating with each other. Simply substituting a healing practice such as massage for a medication does not make for good care. The complementary practice must be integrated properly into your treatment to be safe and effective. Sometimes, you need to act like a good quarterback to make sure your health care team is providing you with treatments that are complementary and not redundant or harmful.
Communicating with Your Doctor
In this day of 15- or 20-minute office visits, many physicians find themselves rushing from exam room to exam room without time to even take a breath. This can make it difficult to spend the time required to manage chronic pain. Here are some strategies to make it easier on both of you.
- Write down your concerns before your visit.
- Stay focused on one thing that’s bothering you. Is it that you can’t sleep because of the pain? You can’t play with your children? You are missing work? Tell your doctor what matters to you in addition to what’s the matter.
- Describe the pain precisely. Saying “it hurts” doesn’t help. Many clinicians use a 1-10 pain scale, with 10 being the worst pain you’ve ever felt and one being no pain. A more helpful way to describe your pain is to put it into perspective in terms of your normal life. For instance, “I used to be able to walk up and down six flights of stairs with no problem; now I have to take the elevator.”
- Track your pain. For a week before your visit, keep a pain diary in which you rate your pain every couple of hours on a scale of 1 to 10 and what you were doing. Also track all pain medications you take. Write down any non-medical approaches you use to cope with your pain.
- Take advantage of your pharmacist if you have medication-related questions. They are knowledgeable about medications, how well they work, and side effects.
- Be honest with your health care provider in terms of alcohol and drug use, diet, exercise, and other providers you’ve seen.
- Bring a friend or family member to your appointment who can take notes. If you are in pain and/or nervous, you may forget things.
YOUR RIGHTS AND RESPONSIBILITIES AS A PERSON WITH PAIN
As someone with pain, you have certain rights and responsibilities when interacting with the health care system.
You have the right to:
- Have your pain taken seriously.
- Be treated with respect.
- Have your pain evaluated holistically, based on its impact on your life, not just on the injury or medical condition.
- Understand why you have pain.
- Receive education about your pain and treatments.
- Be included in any treatment decisions.
- Refuse any treatment (i.e., opioids, additional and/or repeated tests, procedures and surgeries).
- Receive evidence-based care. For instance, there is no evidence that bed rest helps with back pain; in fact, it’s one of the worst things you can do for it. 24
But you are also responsible for:
- Treating your health care team with respect.
- Communicating your goals and values as they relate to the pain. For instance, it might be most important that you return to playing tennis, even if you have some residual pain.
- Following the treatment plan you and your health care provider agree upon, including your self-management regiments.
- Telling your health care practitioner when something isn’t working, or if you’re having side effects.
- Knowing what your insurance covers, which providers are in network, and if you need pre-authorizations for treatment.
- Having realistic expectations. For instance, you may never find a “cure” for your pain. Instead, you can shift your perspective and work with health care professionals to learn how to manage your pain.
Pain in Kids
Children and adolescents also can experience chronic pain, most commonly headaches and abdominal pain. They are often treated with pain medication, even though there are few studies of these drugs in children. However, non-drug approaches have been shown to have a positive and long-lasting impact, including guided imagery in which children listen to an audio recording that helps them envision pleasant experiences, meditation and other relaxation techniques, biofeedback, yoga, and cognitive behavioral therapy, in which they learn to change their thinking around their pain. 25-30
While there are pediatric pain specialists, they are few and far between. Instead, work with your child’s primary care physician and other specialists, such as neurologists and gastroenterologists, as well as non-physician providers such as chiropractors and acupuncturists.
MAKE THE MOST OF YOUR INSURANCE COVERAGE
Here are a few things you can do if your health insurance company denies your claim or requires that you
first use opioids to treat your pain:
- Know your benefits. Before you make an appointment for a treatment, check to see if your insurance covers it.
- Obtain all necessary pre-authorizations before undergoing any procedures.
- Appeal the decision and get your doctor to write a note. If it’s denied, appeal again. There are often several levels of appeals.
- Talk to someone in your company’s human resources; they may be able overrule any insurance decision in large companies that are self-insured – meaning they pay claims directly.
Check to see if you have a health savings account or flexible savings account, which allow you to use pre-tax dollars to pay for non-covered health care costs.
CONNECT WITH OTHERS LIVING WITH CHRONIC PAIN
Look for organizations that support people living with pain and/or people with your particular pain condition. Networking with others who have similar symptoms or access the same health care services has many benefits.
- Networking with people who live with similar symptoms lets you know you are not alone.
- Hearing the variety of tools used by other people with pain may give you some ideas of other options to discuss with your health care team.
- Learning about research pertinent to your symptoms or condition.
- Accessing references and resources on your own schedule.
CONCLUSION
Chronic pain is a complicated, challenging medical condition. Managing your pain while navigating the health system can feel overwhelming. But you can lessen the strain by working with the right providers, knowing your rights, and making the most of your health care coverage.
Focus on building a strong patient-doctor relationship – one that helps you improve your quality of life. For those looking to move away from opioids, remember that there are effective, accessible, non-drug options. With the right team supporting you, you can be in control of your own path to healing.
RESOURCES
- American Society of Regional Anesthesia and Pain Medicine
- American Academy of Integrative Pain Management
- American Academy of Pain Medicine
- American Chronic Pain Association
- Partners for Understanding Chronic Pain
- National Center for Complementary and Integrative Health—Pain
- International Pain Foundation
- National Fibromyalgia & Chronic Pain Association
- For Grace
- The Pain Community
- U.S. Pain Foundation
REFERENCES
- Manchikanti L, Singh V, Helm S, 2nd, et al. An introduction to an evidence-based approach to interventional
techniques in the management of chronic spinal pain. Pain Physician. 2009;12(4):E1-33. - Nahin RL. Estimates of pain prevalence and severity in adults: United States, 2012. J Pain. 2015;16(8):769-780.
- Institute of Medicine. Relieving Pain in America: A Blueprint for Transforming Prevention, Care, Education, and Research. 2011.
- Dewar AL, Gregg K, White MI, Lander J. Navigating the health care system: perceptions of patients with chronic
pain. Chronic Dis Can. 2009;29(4):162-168. - Green CR, Anderson KO, Baker TA, et al. The unequal burden of pain: confronting racial and ethnic disparities in
pain. Pain Med. 2003;4(3):277-294. - Schafer G, Prkachin KM, Kaseweter KA, Williams AC. Health care providers’ judgments in chronic pain: the influence of gender and trustworthiness. Pain. 2016;157(8):1618-1625.
- Mezei L, Murinson BB, Johns Hopkins Pain Curriculum Development T. Pain education in North American medical schools. J Pain. 2011;12(12):1199-1208.
- Centers for Disease and Control. Drug overdose deaths in the United States continue to increase in 2015. 2017;
https://www.cdc.gov/drugoverdose/epidemic/index.html. Accessed September 20, 2017. - Chou R, Turner JA, Devine EB, et al. The effectiveness and risks of long-term opioid therapy for chronic pain: a systematic review for a National Institutes of Health Pathways to Prevention Workshop. Ann Intern Med. 2015;162(4):276-286.
- Centers for Disease Control and Prevention. Guideline for Prescribing Opioids for Chronic Pain: Recommendations. 2017.
- Breuer B, Cruciani R, Portenoy RK. Pain management by primary care physicians, pain physicians, chiropractors,
and acupuncturists: a national survey. South Med J. 2010;103(8):738-747. - Townsend CO, Kerkvliet JL, Bruce BK, et al. A longitudinal study of the efficacy of a comprehensive pain rehabilitation program with opioid withdrawal: comparison of treatment outcomes based on opioid use status at admission. Pain. 2008;140(1):177-189.
- Frank JW, Carey EP, Fagan KM, et al. Evaluation of a Telementoring Intervention for Pain Management in the
Veterans Health Administration. Pain Medicine (Malden, Mass). 2015. - Desko L, Nazario M. Evaluation of a clinical video telehealth pain management clinic. J Pain Palliat Care Pharmacother. 2014;28(4):359-366.
- Eisenberg DM, Buring JE, Hrbek AL, et al. A model of integrative care for low-back pain. Journal Of Alternative And Complementary Medicine (New York, NY). 2012;18(4):354-362.
- Gatchel RJ, McGeary DD, McGeary CA, Lippe B. Interdisciplinary chronic pain management: past, present, and future. The American Psychologist. 2014;69(2):119-130.
- Stanos S. Focused review of interdisciplinary pain rehabilitation programs for chronic pain management. Current Pain And Headache Reports. 2012;16(2):147-152.
- Qaseem A, Wilt TJ, McLean RM, Forciea MA. Noninvasive Treatments for Acute, Subacute, and Chronic Low Back
Pain: A Clinical Practice Guideline From the American College of Physicians. Ann Intern Med. 2017;166(7):514-
530. - Martin BI, Gerkovich MM, Deyo RA, et al. The association of complementary and alternative medicine use and health care expenditures for back and neck problems. Med Care. 2012;50(12):1029-1036.
- Relief for your aching back: what worked for our readers. Consum Rep. March 17, 2017. http://www.consumerreports.org/cro/2013/01/relief-for-your-aching-back/index.htm. Accessed June 12, 2017.
- Vickers AJ, Cronin AM, Maschino AC, et al. Acupuncture for chronic pain: individual patient data meta-analysis. Arch Intern Med. 2012;172(19):1444-1453.
- American Massage Therapy Association. Consumer Views & Use of Massage Therapy. 2017; https://www.amtamassage.org/research/Consumer-Survey-Fact-Sheets.html. Accessed June 7, 2017.
- Morley S, Williams A, Hussain S. Estimating the clinical effectiveness of cognitive behavioural therapy in the
clinic: evaluation of a CBT informed pain management programme. Pain. 2008;137(3):670-680. - Dahm KT, Brurberg KG, Jamtvedt G, Hagen KB. Advice to rest in bed versus advice to stay active for acute low-back pain and sciatica. The Cochrane database of systematic reviews. 2010(6):Cd007612.
- Schurman JV, Kessler ED, Friesen CA. Understanding and treatment of chronic abdominal pain in pediatric primary care. Clin Pediatr (Phila). 2014;53(11):1032-1040.
- O’Donnell FT, Rosen KR. Pediatric pain management: a review. Mo Med. 2014;111(3):231-237.
- Landry BW, Fischer PR, Driscoll SW, et al. Managing Chronic Pain in Children and Adolescents: A Clinical Review. PM & R : the journal of injury, function, and rehabilitation. 2015;7(11 Suppl):S295-315.
- Jastrowski Mano KE, Salamon KS, Hainsworth KR, et al. A randomized, controlled pilot study of mindfulness-based stress reduction for pediatric chronic pain. Altern Ther Health Med. 2013;19(6):8-14.
- Fisher E, Heathcote L, Palermo TM, de CWAC, Lau J, Eccleston C. Systematic review and meta-analysis of
psychological therapies for children with chronic pain. J Pediatr Psychol. 2014;39(8):763-782. - Weydert JA, Shapiro DE, Acra SA, Monheim CJ, Chambers AS, Ball TM. Evaluation of guided imagery as treatment
for recurrent abdominal pain in children: a randomized controlled trial. BMC Pediatr. 2006;6:29-29. - Keshavan Meghana. Your mind can be trained to control chronic pain. But it will cost you. Stat. May 30, 2017.
Accessed September 15, 2017. - Foundation KF. Medicaid Benefits. 2015; http://www.kff.org/medicaid/state-indicator/physical-therapy-services/?currentTimeframe=0&selectedRows=%7B%22wrapups%22:%7B%22united-states%22:%7B%7D%7D%7D&sortModel=%7B%22colId%22:%22Location%22,%22sort%22:%22asc%22%7D. Accessed September 21, 2017.
- Health and Human Services. National Pain Strategy. 2017.
- Jacobs H. Pain doctors: Insurance companies won’t cover the alternatives to opioids. Business Insider. August 10, 2016. http://www.businessinsider.com/doctors-insurance-companies-policies-opioid-use-2016-6. Accessed September 18, 2017.
- Thomas K, Ornstein C. Amid Opioid Crisis, Insurers Restrict Pricey, Less Addictive Painkillers. New York Times. September 17, 2017. https://www.nytimes.com/2017/09/17/health/opioid-painkillers-insurance-companies.html?mcubz=3&_r=0. Accessed September 21, 2017.
- Schatman ME, Webster LR. The health insurance industry: perpetuating the opioid crisis through policies of cost containment and profitability. J Pain Res. 2015;8:153-158.
CONTRIBUTORS
Contributors advised the creation of this paper, but the product is the work of the author and not necessarily a reflection of the contributors nor their organizations.
Maggie Buckley, MBA
Board of Directors, The Pain Community (paincommunity.org)
Buckley has been a volunteer patient advocate for more than 20 years while living with the chronic pain condition Ehlers-Danlos Syndrome.
Cynthia Toussaint
Founder and Spokesperson, For Grace, forgrace.org
Toussaint has been a leading voice for women living with chronic pain since 2002. She has been living with Complex Regional Pain Syndrome and several other auto-immune conditions for 35 years.
ABOUT THE AUTHOR – DR. WAYNE JONAS
Dr. Jonas is a practicing family physician, an expert in integrative health and whole person care delivery, and a widely published scientific investigator. Dr. Jonas is the president of Healing Works Foundation. Additionally, Dr. Jonas is a retired lieutenant colonel in the Medical Corps of the United States Army.
Dr. Jonas was the director of the Office of Alternative Medicine at the National Institutes of Health (NIH) from 1995-1999, and prior to that served as the Director of the Medical Research Fellowship at the Walter Reed Army Institute of Research. He is a Fellow of the American Academy of Family Physicians.
His research has appeared in peer-reviewed journals such as the Journal of the American Medical Association, Nature Medicine, Journal of Family Practice, Annals of Internal Medicine, and The Lancet. Dr. Jonas received the 2015 Pioneer Award from the Integrative Healthcare Symposium, the 2007 America’s Top Family Doctors Award, the 2003 Pioneer Award from the American Holistic Medical Association, the 2002 Physician Recognition Award of the American Medical Association, and the 2002 Meritorious Activity Prize from the International Society of Life Information Science in Chiba, Japan.
Topics: Acupuncture | Back Pain | Behavior & Lifestyle | Chronic Pain | Inflammation | Pain | Pain Management | Self-Care | Social Support
